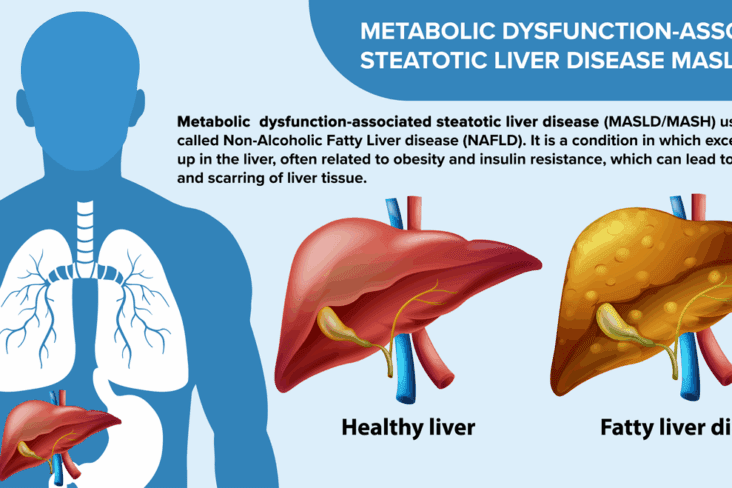
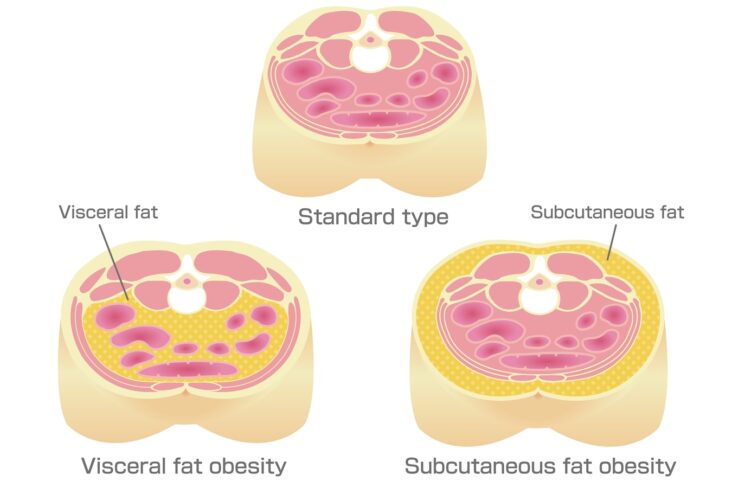
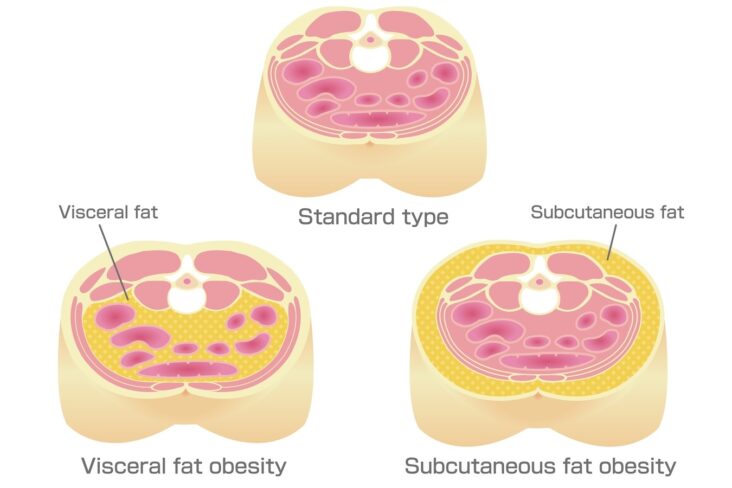
How to Reduce Visceral Fat Without Medication
The most effective path to reducing visceral fat without medication is not just to “eat less.” It’s to build more muscle, eat smarter, and track your progress. In this blog, which also forms one of the chapters of an ebook, I outline the programme and tools our patients use in our cardiometabolic clinic.