Written by Dr Edward Leatham, Consultant Cardiologist
What is a heart attack — and why understanding the causes matters
A heart attack happens when blood flow to part of the heart muscle is suddenly reduced or blocked, causing damage to the heart.
Most people associate heart attacks with blocked arteries, and this is correct in many cases — but it is not the only explanation. Heart rhythm problems, heart muscle diseases, blood clots, and even severe stress can all lead to sudden heart injury.
Understanding the different causes can help people recognise risk earlier, seek medical advice sooner, and in many cases prevent serious problems.
⭐ Key Points
- Most heart attacks are caused by blocked coronary arteries.
- Some occur because of heart rhythm or heart muscle conditions.
- Many risk factors can be detected early and managed effectively.
A. Blocked Arteries and Blood Clots
Coronary Heart Disease (the most common cause)
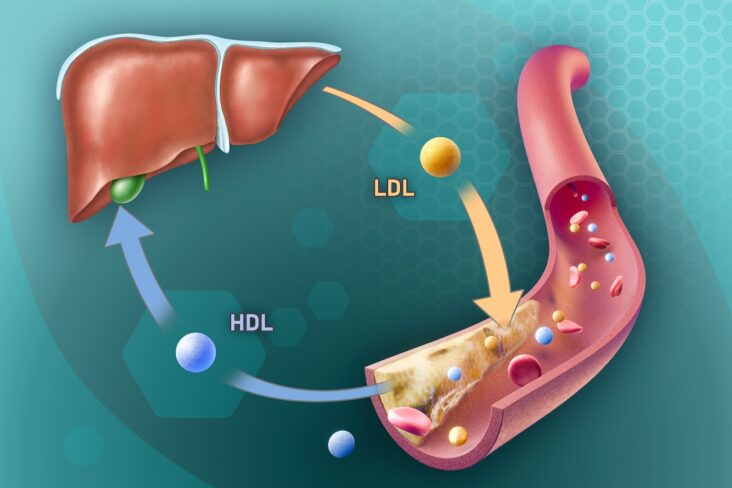
Coronary heart disease develops when fatty deposits build up inside the heart’s arteries. Over time, these arteries narrow and blood flow is reduced.
A heart attack happens when a blood clot forms on top of this build-up and suddenly blocks the artery.
The challenge is that coronary heart disease can develop silently for many years. For some people, the first sign may unfortunately be a heart attack. The good news is that modern scanning, risk assessment, and lifestyle changes can help identify and reduce risk early.
Embolism from Atrial Fibrillation
Atrial fibrillation (AF) is a common condition that causes an irregular heartbeat. When the rhythm is irregular, blood can collect inside the heart and form clots.
Rarely, a clot can travel and block a heart artery, leading to a heart attack.
Many people with AF have no symptoms, which is why simple pulse checks or ECG monitoring — especially over the age of 50 — can be very helpful.
Spontaneous Coronary Artery Dissection (SCAD)
SCAD is a less common cause of heart attack but is being recognised more often, particularly in younger individuals and women who may otherwise be healthy.
It happens when a small tear develops in the wall of a coronary artery, reducing blood flow to the heart muscle.
Although uncommon, outcomes are often good when recognised and managed appropriately.
B. Conditions That Strain or Weaken the Heart
Pulmonary Embolism
A pulmonary embolism is a blood clot that travels to the lungs, usually from the legs. While it is not a classic heart attack, it places sudden strain on the heart.
In severe cases, this strain can cause heart failure or significant heart damage.
People with a family history of blood clots should discuss risk assessment with their doctor, as preventative treatment can be very effective.
Long-Standing High Blood Pressure
High blood pressure forces the heart to work harder over many years. This extra workload can gradually weaken the heart muscle and lead to heart failure.
When the heart is already under strain, it becomes more vulnerable to damage during other cardiac events.
Regular blood pressure checks are one of the simplest and most effective ways to reduce future risk.
Viral Myocarditis (Inflammation of the Heart)
Some viral infections can cause inflammation of the heart muscle, known as myocarditis.
This can temporarily weaken the heart and cause chest pain, breathlessness, or palpitations. Most people recover well, but early diagnosis is important and may involve ECGs, blood tests, heart ultrasound, and cardiac MRI.
C. Heart Muscle Diseases (Cardiomyopathies)
Cardiomyopathy simply means disease of the heart muscle. These conditions can weaken the heart or increase the risk of dangerous heart rhythms.
Hypertrophic Cardiomyopathy
This inherited condition causes the heart muscle to become abnormally thick. In some people it increases the risk of rhythm problems and sudden cardiac events.
Because it can run in families, screening may be recommended when there is a history of heart disease or sudden collapse.
Dilated Cardiomyopathy
In dilated cardiomyopathy, the heart becomes enlarged and weaker, making it harder to pump blood effectively.
It may be caused by genetics, previous viral infections, alcohol, or other factors. Treatment can significantly improve symptoms and long-term outlook.
Other Cardiomyopathies
Less common forms include restrictive or arrhythmogenic cardiomyopathy, where the heart becomes stiff or prone to abnormal rhythms.
Although these conditions are rarer, specialist assessment and monitoring can greatly reduce risk.
Takotsubo Cardiomyopathy (“Broken Heart Syndrome”)
This condition is triggered by intense emotional or physical stress and causes temporary weakening of the heart muscle.
It feels very similar to a heart attack and always needs urgent assessment, but most people recover well over time.
D. Electrical Problems of the Heart
Long QT Syndrome and Brugada Syndrome
These are inherited conditions affecting the heart’s electrical system. They can lead to dangerous heart rhythms and, rarely, sudden cardiac arrest.
Although uncommon, they are important because many people are otherwise healthy before diagnosis. Specialist cardiology assessment can identify and manage these conditions effectively.
When Should You Seek Urgent Help?
You should seek emergency medical attention if you experience:
- Chest pressure, tightness, or pain lasting more than a few minutes
- Sudden shortness of breath
- Unexplained collapse or fainting
- New severe or rapid palpitations
- Sudden sweating, nausea, or feeling unwell with chest symptoms
It is always safer to get checked early.
Three Simple Things You Can Do Today
- Know your blood pressure and have it checked regularly
- Pay attention to your pulse and heart rhythm
- Seek assessment if you develop new or changing symptoms
Final Thoughts
Heart attacks can happen for several different reasons, not just blocked arteries. The encouraging news is that many causes can be recognised early and treated successfully.
Regular health checks, awareness of symptoms, and early medical assessment can make a major difference — helping people stay healthy and active for longer.