Prologue: A Cardiologist’s and Nutritional Therapist’s Perspective
Written by Dr Edward Leatham, Consultant Cardiologist and Juliette Martin Nutritional Therapist
As clinicians with a scientific background, there is an expectation by patients and peers that we sift through scientific literature and medical research with a critical eye to spot medical misinformation and unsubstantiated treatment strategies. Our role is to guide patients towards evidence-based treatments that could help them feel better and live longer, healthier lives. We must also be mindful of past treatment fads that became popular through collective enthusiasm and clever marketing, only years later to be found to be causing harm.
Recently, a surge in queries from heart patients about glucose monitoring (used in Zoe and Veri Apps) and the use of artificial intelligence (AI) to guide lifestyle and food intake has led us to delve deeper into the science behind the widely quoted assertion that glucose spikes are harmful. This article aims to provide an overview of some fairly convincing, yet still largely unexplored evidence of potential harm caused by glucose spikes, particularly in relation to harmful glycosylation of tissues and increased oxidative stress. It also serves as a reminder to our patients that most clinicians still await evidence from properly randomised controlled clinical trials, before recommending that reducing glucose spikes per se, will always lead to long-term benefit.
Based on existing guidelines supported by a strong medical evidence base, there is certainly nothing wrong with encouraging our patients to follow a diet and lifestyle aimed at lowering glucose and promoting weight loss. Making use of all of the information we can glean using the latest technology, we support early adoption, provided that patients are clear that the widely circulated claims around benefits achieved by solely reducing glucose spikes have yet to be formally substantiated by large clinical trials.
The Glucose Thermostat: A Precarious Balance
Our bodies possess a sophisticated mechanism for managing glucose levels. Following a meal, carbohydrates are broken down into simple sugar molecules: glucose. This glucose is then circulated throughout the body via the bloodstream. An essential fuel for every cell, glucose must traverse the blood to satiate energy-hungry cells. Herein lies the conundrum: while glucose is necessary, an excess can cause problems. The body must strike a delicate balance, ensuring that blood sugar levels are neither too high (hyperglycemia) nor too low (hypoglycemia).
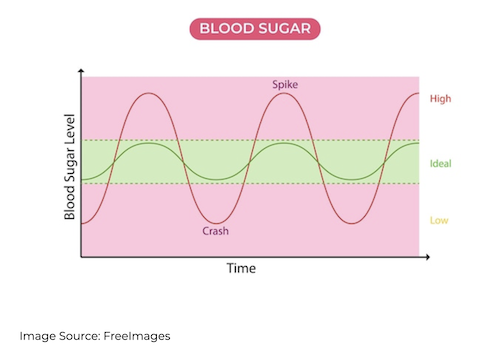
The Hyperglycemia Hazard: The Role of Glucose Spikes
When blood sugar levels are consistently high, causing prediabetes and diabetes, the risk of conditions such as heart disease and type 2 diabetes increase in the long-term. It is easy to understand why the phenomenon of glucose spiking, where blood sugar levels surge and then fall back into the normal range after a meal, is also widely considered to be harmful. While some fluctuation in blood glucose is not only normal but also necessary as the body responds to food intake, it seems logical that as these glucose spikes become larger and a more regular occurrence, that the danger of developing a range of diseases, including diabetes and heart disease, also rises.
Glucose Spikes and Heart Health: Unveiling the Connection
Numerous studies have established a strong link between poor blood sugar responses and an increased risk of heart disease. This is possibly because glucose spikes can interfere with the endothelium’s ability to dilate blood vessels, affecting blood circulation and increasing the risk of plaque formation. Over time, this may accelerate atherosclerosis and, consequently, heart disease. Elevated levels of glucose can also induce inflammation, a key contributor to chronic diseases like type 2 diabetes, some cancers, and heart disease. An attractive, yet unproven hypothesis is that glucose spikes either cause or are associated with coronary artery inflammation which accelerates toxic Apolipoprotein B build up at key focal points in the coronary tree. This might explain the unassailable benefits of both LDL-lowering statins and reduced carbohydrate intake in patients with established coronary heart disease.
The Glucose Paradox: A Puzzle for Medical Science
Interestingly, while a direct correlation has been established between high glucose levels and an increased risk of cardiovascular disease (CVD), there is still debate over whether glucose-lowering treatment directly reduces CVD. This is often referred to as the glucose paradox. Despite this, the evidence that high glucose levels could potentially contribute to CVD is compelling. Postprandial spikes of high glucose levels, in particular, appear to be a significant determinant of CVD risk, however there are not yet any long-term controlled trials in this area to convince the medical world that simply ‘flattening one’s glucose’ curve always leads to long term benefit. Therefore, while we might remain optimistic about this potential benefit, we also need to be cautious about the precise way in which a ‘glucose curve flattening’ outcome is achieved. If our patients reach this goal through increased exercise, a healthier BMI through portion control, reduced consumption of refined carbohydrates, increased fibre intake, stress management and better sleep, we can feel confident of a net gain. However, if glucose curve flattening results are achieved using less healthy dietary ‘hacks’, such as an increase in alcohol, saturated fat and protein intake – specifically from red or processed meats- , or possibly taking novel drugs for which we have no long term outcome data, without due attention to other key factors involved, we should be guarded, at this point, in promising longer-term benefits.
Continuous Glucose Monitors: A Health tech Revolution
The advent of continuous glucose monitors has been a game-changer in this context. These devices, which provide frequent readings of tissue glucose concentrations, have revealed that glucose dysregulation is more common than previously thought. They have also shed light on how specific foods can trigger glucose spikes, helping individuals to steer clear of particularly “spikey” foods and, no doubt, will lead to a plethora of long-term clinical trials required to convince the wider medical profession of a significant health benefit, especially in regard to non-diabetic populations. Since many non-diabetics can also experience hyperglycemia, marked by high fasting blood sugar over 6 mmol/L and elevated readings over 7.8 -10 mmol/L after eating, the ‘off label’ use of CGM (which are currently only licensed for use in diabetics) will initially only be for those at highest cardiovascular risk, along with enthusiasts and early adopters, hopeful of a win, rather than the general population. Symptoms of high blood sugar in non-diabetics may take months or even years to manifest, underscoring why there might be a larger interest in metabolic health than just our patients with prediabetes or diabetes.
Dietary Decisions: The Role of Food Choices in Blood Sugar Levels
Diet plays a crucial role in managing blood sugar levels. Foods high in refined carbohydrates, processed foods,and added sugar are more likely to spike blood sugar levels. Additionally, meal timing can significantly impact postprandial glucose metabolism. Paying attention to not just what you eat but when you eat can be a significant component in stabilising blood glucose.

The Genetic Glucose Factor, sleep, and Stress
Genetics also plays a part in blood sugar regulation. If metabolic dysfunction, insulin resistance and diabetes runs in your family, you may be at greater risk of developing non-diabetic hyperglycemia. Poor sleep and stress are linked to cortisol responses. Therefore, it is clear that, with the right lifestyle habits and food choices, those people that are found to have glucose spikes can significantly reduce these and maintain healthier glucose levels by carefully considered strategies. They do so in the, not unreasonable, hope that this will delay or even prevent the onset of future pre-diabetic and diabetic states.
The Conclusive Verdict: Navigating the Glucose Spikes Conundrum
In conclusion, while glucose spikes could be unhealthy, particularly with regards to harmful glycosylation of tissues and increased oxidative stress, the jury is still out on whether preventing glucose spikes will always lead to better health in the long-term. What is clear is that more information about the impact of our dietary choices on how what we consume affects our blood glucose is certainly insightful and could potentially help individuals lose weight and achieve better overall health outcomes
Epilogue: A Cardiologist and Nutritional therapist recommendations
We support the use of ‘off licence’ glucose monitors for non-diabetic patients under strict medical care with support from a nutritional therapist. Given sufficient information about food intake through food diaries, and with enough background information about medication, lipid profile, sleep, stress, weight, family history, consideration of other medical conditions, this information can be used in our metabolic health assessment, along with insights gleaned from glucose monitoring, to advise our patients.
Overall, while glucose spikes could potentially be harmful, it is crucial to remember that this is simply one piece of the puzzle. A holistic approach to health, encompassing a balanced diet, regular exercise, adequate sleep, and stress management, is key to maintaining optimal well-being and mitigating the risk of diseases such as coronary heart disease.
Further reading
Biofeedback: CGM metrics improve after just 4 weeks of dietary intervention
Metabolic Health Assessment