Written by Dr Edward Leatham Consultant Cardiologist
Image Source: FreeImages
Introduction
Cardiovascular Disease (CVD) remains a significant health concern across the globe. With a vast proportion of the population affected, research into the most effective treatments and preventative measures is paramount. One area of recent breakthrough is the discovery of the role of Proprotein convertase subtilisin/kexin type 9 (PCSK9) in the regulation of low-density lipoprotein cholesterol (LDL-C), often referred to as ‘bad cholesterol’. Interestingly, this discovery was facilitated by the identification of gain-of-function mutations, which are alterations in the human genetic code that increase the normal activity of a gene. The mutations in the PCSK9 gene result in high LDL cholesterol levels and, thus, increase the risk of developing coronary artery disease.
This article looks into the role of PCSK9, the development of PCSK9 inhibitors, their efficiency, and their potential as a game-changer in the management of cardiovascular diseases. It provides a short exploration of the subject, drawing upon the most recent and relevant research and guidelines.
PCSK9: A Key Player in LDL-C Regulation
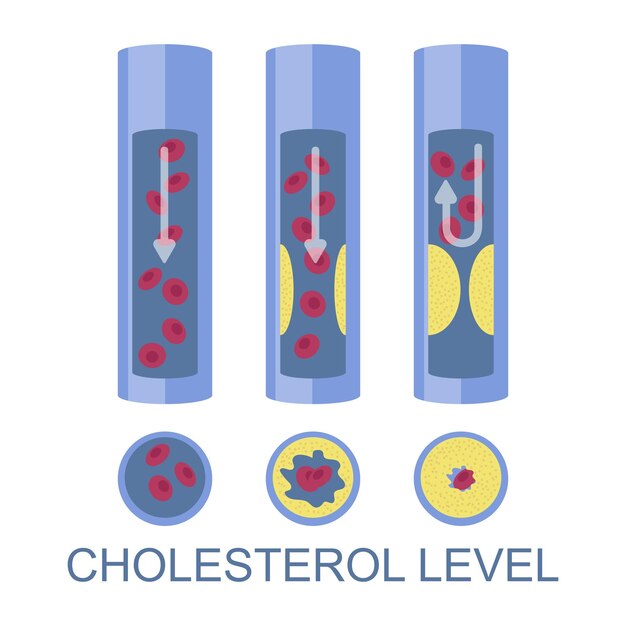
The PCSK9 gene plays a vital role in cholesterol metabolism, specifically in the regulation of LDL receptor degradation. LDL receptors are instrumental in controlling the quantity of LDL cholesterol in our bloodstream. The PCSK9 protein, which is produced in our liver, breaks down these receptors, thus reducing their numbers. Consequently, an increased presence of PCSK9 protein in our bodies leads to fewer LDL receptors in our liver and higher LDL cholesterol levels.
This understanding has provided the basis for the development of PCSK9 inhibitors. These are monoclonal antibodies that prevent the PCSK9 protein from functioning. This intervention leads to an increase in LDL receptors with subsequent decrease in LDL cholesterol levels. With lower PCSK9 levels available to internalise LDL receptors, the liver becomes a great deal more effective in clearing LDL from the circulation. When used with statins, these new therapies lead to an astonishing reduction in serum LDL. Once long term safety is established in larger populations it is likely we will see a major expansion in these drugs as they are convenient to take, are associated with few side effects and, unlike statins, appear to restore the liver’s natural LDL lowering action by overriding common gain of function mutations that lead to increased PCSK9 pathway activity.
PCSK9 Inhibitors: A New Era in Cholesterol Management
In 2015, the FDA approved two PCSK9 inhibitors, alirocumab (Praluent) and evolocumab (Repatha). These drugs work by a pathway that is distinct from the one used by statin medications, and they can be used in conjunction with statins for a more substantial reduction in LDL cholesterol levels.
PCSK9 inhibitors are typically administered by injection, with dosages varying between every two to four weeks. These inhibitors have shown significant efficiency in reducing LDL cholesterol levels, with some studies reporting average LDL cholesterol reductions of 60%.
Cardiovascular medicine has now also entered an era of RNA therapeutics. It is now possible to selectively target genes that have key roles in lipid metabolism by antisense oligonucleotides and small interfering RNA (siRNA). One such siRNA, called inclisiran, targets the PCSK9 gene and has shown promising results in clinical trials. It has a more prolonged LDL-lowering efficacy than PCSK9 inhibitors, which permit it to be administered less frequently. In 2023 NHSE and NICE approved the use of Inclisiran for patients unable to tolerate orally active lipid lowering drugs such as Statins, Ezetimibe and bempedoic acid.
Who Can Benefit from PCSK9 Inhibitors?
The latest cholesterol treatment guidelines recommend PCSK9 inhibitors as a potential treatment for individuals with high risk of CVD. This high-risk group includes individuals with known CVD or those with elevated cholesterol levels and diabetes. For these individuals, the guidelines recommend an LDL cholesterol target of less than 1.8 mmol/L (<70 mg/dl).
Initial studies have shown that PCSK9 inhibitors, when compared against placebo, demonstrated robust reductions in CVD events. Furthermore, a 2019 study published in JAMA Cardiology found that adding a PCSK9 inhibitor to a statin in patients with stable CVD and elevated LDL cholesterol levels (greater than 70 mg/dl) significantly reduced future CVD events.
Side Effects and Cost of PCSK9 Inhibitors
Like all medications, PCSK9 inhibitors are associated with potential side effects. These may include flu-like symptoms, fatigue, back pain, and muscle aches. The most common side effect reported is pain at the injection site. However, these inhibitors are generally well-tolerated.
The cost of PCSK9 inhibitors was initially high, but prices have significantly decreased in the recent past. Prescription coverage has also broadened to include these medications, although restrictions apply based on individual plans
Comparison of PCSK9 Inhibitors and Statins
Both PCSK9 inhibitors and statins are commonly used in the management of high LDL cholesterol levels. Statins work by blocking an enzyme in the liver that is responsible for making cholesterol. They help the body reabsorb built-up cholesterol deposits from the arteries, thereby reducing the amount of cholesterol in the blood.
By contrast, PCSK9 inhibitors work by blocking the PCSK9 protein, which increases the number of LDL receptors in the liver and accelerates the clearance of LDL cholesterol from the bloodstream.
While both drugs are effective, some individuals might not be able to tolerate statins due to side effects such as muscle pain and digestive problems. In such instances, PCSK9 inhibitors may provide a valuable alternative.
Future Perspectives
Exciting developments in the field of PCSK9 inhibitors offer promising avenues for future research. The advent of gene editing using CRISPR-Cas9 has opened up the possibility of permanently altering genes, including the PCSK9 gene This could prove revolutionary for diseases caused by elevated LDL-C, such as atherosclerosis.
Conclusion
PCSK9 inhibitors represent a significant advancement in the management of cardiovascular disease. They provide an effective alternative for individuals who are unable to tolerate statins or have not achieved the desired LDL cholesterol levels with conventional treatments. As research continues, it is likely that our understanding of the role of PCSK9 in cholesterol metabolism will continue to evolve, leading to further advancements in the treatment and prevention of cardiovascular disease.
While the potential benefits of these inhibitors are substantial, it is worth noting that they are not a substitute for statin therapy, a healthy lifestyle. Regular exercise, a balanced diet, and smoking cessation remain the cornerstones of cardiovascular disease prevention.
Chasing LDL cholesterol to the bottom — PCSK9 in perspective
PCSK9 inhibition: A game changer in cholesterol management
PCSK9 Inhibitors: What You Need to Know
PCSK9 Inhibitors
Association of Triglyceride-Lowering LPL Variants and LDL-C–Lowering LDLR Variants With Risk of Coronary Heart Disease