An article written by Dr Edward Leatham, Consultant Cardiologist © 2024 E.Leatham
For busy people, or to tune in when on the move, Google Notebook AI audio podcast are available for this story beneath.
In today’s world, where the pursuit of a healthy and long life is paramount, the importance of managing blood pressure has become increasingly significant. With an upsurge in patients over 80 experiencing heart failure linked to poorly controlled blood pressure from midlife, it’s crucial that individuals, particularly from the age of 40 upwards, pay close attention to their blood pressure readings to foster a healthy aging process.
When blood pressure hovers at the borderline, many patients hesitate to start medication. This reluctance has spurred interest in non-pharmacological methods to lower blood pressure, aiming to delay the need for pharmaceutical intervention as much as possible for long-term benefits.
One challenge in advocating non-pharmacological approaches is the lack of robust data from randomized controlled trials. Unlike pharmacological studies, these methods don’t involve drug patents, which often leads to less scientific scrutiny. However, this shouldn’t discourage individuals from exploring lifestyle and dietary changes to see if they can effectively manage their blood pressure.
With the advent of accurate home blood pressure monitors, individuals can now undertake personal experiments to assess the impact of various interventions on their blood pressure. This “N of 1” experiment is gaining popularity, offering a personalised approach to managing blood pressure.
The process starts with obtaining a reliable baseline of blood pressure readings, ideally using a quality cuff-based monitor in the morning and evening. By discarding the first reading and focusing on the subsequent ones, individuals can calculate a weekly average that reflects their true blood pressure more accurately.
It is important that your blood pressure is well controlled, and low enough to prevent long term damage to the circulation. The gold standard for diagnosis, recommended by NICE, is ambulatory blood pressure monitoring, however a cost effective alternative is to use an suitable home blood pressure monitor. It is recommended that you purchase or loan an accurate device as recommended by the British Hypertension Society at a cost of between £35-100. There are various sorts, but we have found the most reliable involve a cuff rather than a wrist measurement. If you have a large arm, it is important that you use a large cuff. Ideally the nurse at your GP practice or at our clinic should check the device to make sure it is accurate by taking a manual recording of blood pressure at the same time as recording the pressure on the device.
Rather than take multiple blood pressure recordings throughout each day, which can be confusing as there is much variation, and diurnal variation in blood pressure occurs, it is best that you take the average of recordings taken at the same time every morning and evening, usually shortly after rising or retiring to bed.
Because of variations in machine accuracy and variation in blood pressure during the day, we use a statistical technique known as “regression to the mean” to overcome measurement and machine inaccuracies. The blood pressure should therefore be recorded three times on the trot at the same time every day for 4-7 days.
- Sit at a table with the arm relaxed.
- Three readings should be taken with a few minutes interval between.
- Discard the first, and work out the average for the 2nd and 3rd recording.
- Repeat each day, and then work out the weeks average (see example below) or download our spreadsheet template.
At this point the blood pressure machine can be put away, usually for three months.
There is evidence that if you take it all the time, every day, there is a risk of cardiac neurosis!
You can print off our average sheet or ask your doctor who can send you an spreadsheet template or paper version like this example excel spreadsheet template.
The target blood pressure (average at home) for a non-diabetic patient is < 135/85 mmHg and for a diabetic patient is < 130/80 mmHg.
Upon establishing this baseline, various interventions like diet changes, weight loss, or salt intake reduction can be tested. After a week or so of the intervention, a second set of readings can help determine if the changes have made a significant impact, with a 5 to 8 mmHg reduction in blood pressure being a meaningful improvement.

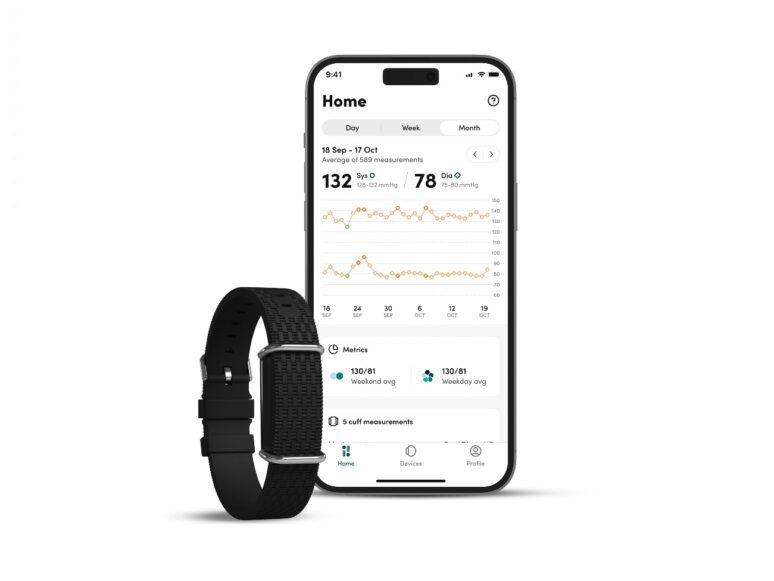
Recently, we have started using and recommending a new technology that measures the blood pressure using a light sensor, calibrated with a cuff. The Aktiia/HiLo system is popular and well validated. New watch systems by other vendors are available in late 2024.
You should discuss the results with your GP or Specialist.
Conclusion
In summary, it is easy to take your blood pressure at home using these guidelines. Due to the high incidence of HFpEF and stiff heart in old age, everyone interested in a healthy retirement years should ‘know their BP numbers ‘ from their mid 30s onwards.
Key messages
- When it comes to heart failure, stroke and dementias, your blood pressure is considered to be a modifiable major risk factor.
- If you have raised blood pressure, once equipped with a BP measuring strategy and a little know how you can try out your own N of 1 trial to assess whether lifestyle measures such as weight reduction, salt, alcohol reduction and an increase in exercise can get you to target before even considering medication.
- If your blood pressure remains over target, go and see a healthcare professional to get a prescription for some medication – well tolerated, extremely well proven and amazingly low cost. It will alter your life!
For other stories related to blood pressure, heart failure, and stroke, explore the archives by entering a tag under the search function above.
Further Reading
- Measuring your BP E-book
- Natural methods to lower your blood pressure
- Why the best blood pressure may be the lowest you can manage without falling over when you stand up!
- Let’s talk about salt: debunking common myths
- Your Blood Pressure
The Naked Heart is an educational project owned and operated by Dr Edward Leatham. It comprises a series of blog articles, videos and reels distributed on Tiktok, Youtube and Instagram aimed to help educate both patients and healthcare professionals about cardiology related issues.
If you would like to receive email notification each week from the Naked Heart, follow me on social media or please feel free to subscribe to the Naked Heart email notifications here